Losing vision in one eye can feel like stepping into a new world—one where depth is uncertain, movement feels unsteady, and everyday tasks suddenly demand intense focus. This condition, known as monocular vision, affects people of all ages due to trauma, surgery, infection, or congenital issues. While not classified as legal blindness, it brings real functional consequences: a 30% loss of peripheral vision and the complete absence of stereoscopic depth perception. Yet, the brain’s ability to adapt through neuroplasticity allows most individuals to regain independence and confidence over time.
Adapting to life with one eye isn’t instantaneous. Most people need six to nine months for initial adjustment, though many continue refining skills for years. Adults who lose binocular vision suddenly face a steep learning curve—relearning how to judge distances, avoid collisions, and even interpret social cues. Children born with monocular vision often adapt seamlessly, but older kids and teens may struggle emotionally and physically after surgery or injury. The good news? With targeted training, protective habits, and peer support, living well with one eye isn’t just possible—it’s achievable. This guide explores science-backed strategies for depth perception, mobility, driving, eye safety, child development, and emotional resilience to help you thrive.
Rebuild Depth Perception Using Monocular Cues

Without input from both eyes, the brain loses stereopsis—the most precise tool for judging distance. But it doesn’t lose all depth perception. Nine monocular cues can compensate when used consciously and consistently.
Use Motion Parallax for Accurate Distance Judgment
As you move your head side to side, closer objects appear to shift faster across your visual field than distant ones. This dynamic cue—similar to how cats sway their heads before jumping—is one of the most effective tools for depth estimation. Practice deliberate head movements when reaching for items, descending stairs, or judging car distances while driving. Even small left-right motions provide critical spatial information that static viewing cannot.
Apply Relative Size and Overlapping Objects
Familiar objects help estimate distance based on size. A car that appears smaller is likely farther away. When one object blocks another—like a chair partially hiding a bookshelf—the blocked object is farther. Train yourself to notice these overlaps, especially in cluttered spaces like kitchens or crowded sidewalks.
Rely on Linear Perspective and Texture Gradients
Parallel lines such as roads, floor tiles, or sidewalk edges converge with distance. The degree of convergence signals how far away something is. Similarly, textures become finer and less detailed as distance increases—a gravel path looks coarse up close but smooth from afar. Use these visual patterns indoors and outdoors to gauge depth more accurately.
Interpret Light, Shadow, and Atmospheric Haze
Shadows reveal an object’s shape and elevation. Brighter surfaces often appear closer due to higher light reflection. For distant views, atmospheric haze (aerial perspective) makes faraway hills look bluer or grayer. These subtle cues help judge terrain during walking, driving, or outdoor navigation.
Improve Daily Coordination and Reduce Accidents
Monocular vision disrupts hand-eye coordination and spatial accuracy. Simple actions like picking up a cup or catching a ball become error-prone. But with consistent practice and tactile feedback, most challenges can be managed.
Increase Accuracy in Reaching and Grasping
Missing targets is common early on. To improve:
- Anchor your hand on a table before setting down a drink.
- Guide with touch: Wrap your non-dominant hand around a cup while pouring.
- Use container edges: Gently tap the lip of a pitcher against the rim of a glass before pouring.
- Slow down: Rushing increases misjudgments. Move deliberately until muscle memory develops.
Occupational therapy focusing on reaching and grasping can significantly reduce errors in just a few sessions.
Navigate Stairs and Curbs Without Falling
Falls are a real risk due to poor depth judgment. Prevent accidents by:
- Feeling with your foot: Test the edge of the next step before committing your weight.
- Use handrails: Always hold the railing, even if it feels unnecessary.
- Look sideways: Turn your head to view steps from an angle, enhancing depth cues.
- Mark step edges: Use contrasting tape on stair nosings for better visibility.
Minimize Spills When Pouring Liquids
Spilling is frustrating but avoidable. Try these techniques:
- Pour slowly and stop frequently to check the liquid level.
- Use clear containers so you can see the fill line.
- Position the receiving cup against your body or a countertop for stability.
- Listen for changes in sound as the cup fills—the noise drops when full.
Master Head Scanning to Compensate for Blind Spots
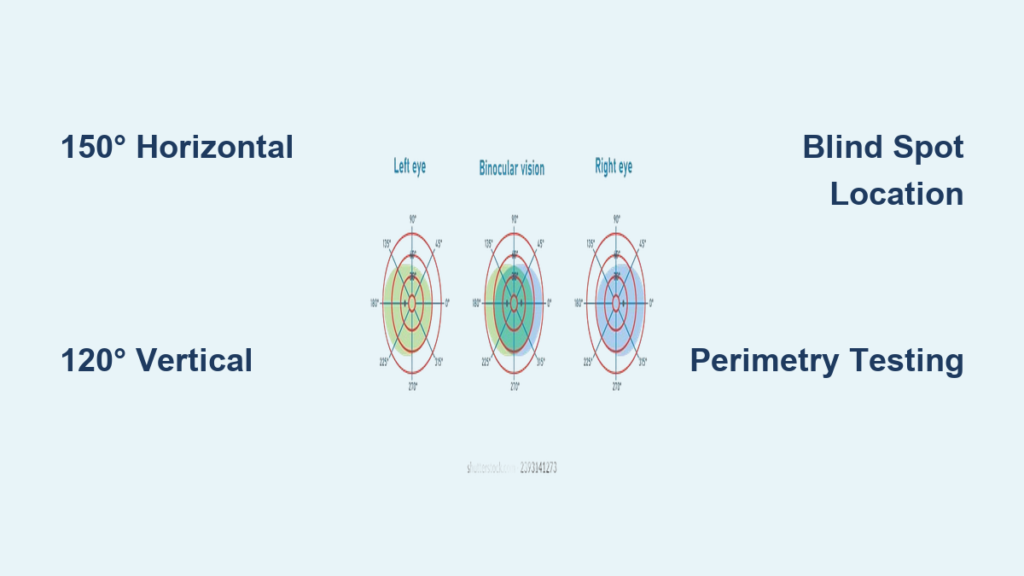
With monocular vision, you have a blind spot of about 30% on the side of vision loss. Passive observation isn’t enough—you must train yourself to scan deliberately.
Scan Before Moving in Crowded Areas
People and objects appear suddenly unless you check first. Make it a habit to:
- Turn your head fully toward the non-seeing side before stepping into crosswalks, doorways, or store aisles.
- Stop and scan before changing direction in busy areas.
- Announce your presence verbally—say “on your left” or “coming through.”
Author Anne Rice, who lost vision after surgery, learned to pause and check her right side before moving in stores—a simple habit that prevented collisions.
Prevent Chronic Neck Pain from Asymmetry
Many unconsciously tilt or rotate their head to maximize input from the seeing eye. Over time, this causes chronic neck strain. Prevent it by:
- Practicing symmetrical posture in front of a mirror.
- Doing daily neck stretches and shoulder rolls.
- Setting phone or computer screens centrally.
- Using reminders (alarms, sticky notes) to correct posture.
If pain persists, consult a physical therapist familiar with visual field compensation.
Drive Safely with One Functional Eye

Driving is permitted for many with monocular vision, provided key criteria are met. Safety depends on adaptation, training, and equipment adjustments.
Meet Legal and Medical Requirements
In the UK, the DVLA requires:
- Visual acuity of 6/12 or better on the Snellen chart in the seeing eye.
- Ability to read a number plate from 20 meters.
- Full visual field in the functioning eye.
- No double vision (diplopia).
- Medical clearance from an ophthalmologist.
You must inform the DVLA of monocular vision. Failure to report can invalidate insurance.
Wait and Train Before Returning to Driving
After sudden vision loss, do not drive for at least three months. This allows neurological adaptation and reduces accident risk. Before resuming:
- Undergo evaluation by an orientation and mobility specialist.
- Practice in low-traffic areas with a trained instructor.
- Get assessed in your own car at familiar locations (e.g., grocery store, church).
Dr. Diane Whitaker’s protocol at Duke Eye Center includes on-road training tailored to individual routines, improving confidence and accuracy.
Enhance Visibility with Mirrors and Head Movement
- Turn your head more: Glance over your shoulder toward the blind side when changing lanes or parking.
- Upgrade mirrors: Install wide-angle or convex side mirrors to reduce blind spots.
- Check twice: Always verify empty zones before maneuvering.
- Avoid high-speed highways initially; build experience gradually.
HGV and PSV drivers must complete a V1V form and may face additional restrictions.
Note: The RNIB cannot approve driving—only medical professionals and licensing agencies can.
Protect Your Remaining Eye at All Costs

Your single functioning eye is irreplaceable. Preventive protection is non-negotiable.
Wear Polycarbonate Lenses Every Day
Even if you don’t need vision correction, wear impact-resistant polycarbonate lenses in sturdy frames. These lenses:
- Withstand high-velocity impacts.
- Block UV radiation.
- Are standard in sports and safety eyewear.
Use plano (non-prescription) lenses if no correction is needed.
Use Safety Goggles for Risky Activities
Engage in DIY, gardening, or crafting? Wear ANSI-approved safety goggles. Common hazards include:
- Flying debris (lawn mowers, drills)
- Chemical splashes
- Dust and particles
Regular glasses—even polycarbonate ones—do not offer full protection.
Avoid High-Risk Sports or Wear Protective Shields
Contact and projectile sports pose serious threats. Avoid:
- Boxing, wrestling, martial arts
- Basketball, football, baseball
- Racquet sports (tennis, squash)
If you choose to play, wear a face shield or protective goggles designed for the sport. Consult an ophthalmologist for recommendations.
Schedule Annual Eye Exams
See an eye specialist at least once a year to detect early signs of:
- Glaucoma
- Cataracts
- Retinal detachment
- Macular degeneration
Early treatment preserves vision and prevents total loss.
Support Children’s Development and Confidence
How children adapt depends on age and timing of vision loss.
Encourage Head Turning in Infants
Babies naturally favor the seeing side. Stimulate head movement by:
- Placing light-up or noisy toys on the blind side.
- Rolling balls or cars across the floor to encourage tracking.
- Holding the child so their seeing eye faces outward, not into your shoulder.
This builds neural pathways for scanning and spatial awareness.
Promote Coordination in Toddlers and Kids
For older children:
- Tape straight lines on the floor and have them walk along them.
- Play catch with large, soft balls.
- Hang targets at varying distances for bean bag throws.
- Position favorite toys higher or farther away to promote reaching.
Avoid handing items directly—encourage reaching to develop eye-hand coordination.
Address Emotional and Social Needs
Older children and teens may feel self-conscious about patches or prosthetics. Talk openly about appearance and reassure them. Ask care teams:
- How long will adjustment take?
- Are there exercises to help?
- What activities should be avoided?
- Is school support available?
Peer interaction and adaptive play accelerate both physical and emotional recovery.
Manage Social Misinterpretations and Build Confidence
Monocular vision affects more than vision—it influences how others perceive you.
Correct Gaze Misunderstandings
People may think you’re staring or not paying attention because the non-seeing eye doesn’t track. Explain gently: “I only see clearly from one side—my eye doesn’t move the same way.”
In group conversations, turn your head fully toward speakers to appear engaged.
Handle Assumptions About Awareness
Friends might say, “You must’ve seen me!” when you didn’t. Respond with clarity: “I have a blind side—I didn’t see you coming from that direction.”
Teach others to approach from your seeing side when possible.
Choose Discreet or Stylish Eye Coverings
Traditional patches can draw unwanted attention. Alternatives include:
- Tinted lenses in regular glasses—one clear, one dark.
- Flush-fitting medical patches (not costume-style).
- Ocular prosthetics after enucleation, which improve symmetry and protect the socket.
Some find confidence in bold designs—patches as fashion statements.
Combat Visual Fatigue and Cognitive Load
Using one eye increases mental effort. The brain works harder to fill in missing data, leading to visual fatigue.
Recognize Signs of Eye Strain
Symptoms include:
- Headaches after reading or screen use
- Difficulty focusing after prolonged tasks
- Irritability or reduced concentration
Fatigue doesn’t damage the eye but impairs performance.
Take Regular Visual Breaks
Follow the 20-20-20 rule:
- Every 20 minutes, look at something 20 feet away for 20 seconds.
Also:
- Dim screens to reduce glare.
- Use large fonts and high contrast.
- Work in well-lit environments.
- Limit screen time during early adaptation.
Rest restores clarity and prevents burnout.
Living with monocular vision is not about returning to “normal”—it’s about building a new normal. The journey involves grief, adaptation, and resilience. But with time, training, and protection, most people not only adjust—they thrive. As one person put it: “This isn’t about fixing a disability. It’s about thriving within it.”